Role of Technology in IVF: Faster, Smarter, and Personalized
- Jan 21
- 18 min read

Confusion about what modern IVF really involves remains common, even as technology transforms fertility care worldwide. For women under 40 with strong ovarian reserve, the gap between myth and reality can mean costly delays and heightened stress. Understanding the true scope of IVF and the role of artificial intelligence—including how it enables rapid, affordable, and more precise treatment—gives you control over your journey. This guide reveals how advanced IVF addresses misconceptions, supports faster decision-making, and keeps the human element at the center of your experience.
Table of Contents
Key Takeaways
Point | Details |
Understanding IVF | In vitro fertilization is a complex, multi-step process that has significantly advanced with technology, specifically through the integration of artificial intelligence and real-time monitoring. |
Avoiding Misconceptions | Common myths about IVF can lead to unnecessary delays and stress; it is essential to understand that success rates vary and technology does not eliminate human oversight. |
Personalization of Treatment | AI-driven personalized protocols not only enhance efficiency but also increase the likelihood of success, making treatment more affordable and tailored to individual needs. |
Emotional and Supportive Care | Effective fertility treatment combines advanced technology with compassionate human support, emphasizing the importance of clear communication and emotional resources throughout the process. |
Defining IVF Technology and Misconceptions
In vitro fertilization has evolved dramatically over the past few decades, transforming from a procedure that seemed almost experimental into a well-established medical treatment. Yet despite its prevalence, significant confusion persists about what IVF actually involves and what modern technology can accomplish. Understanding the true definition of IVF technology and dispelling common myths is essential for anyone considering treatment, particularly women under 40 with healthy ovarian reserve who want to make informed decisions quickly. The gap between perception and reality often leads to unnecessary anxiety, delayed treatment, and costly missteps that extend your timeline and drain your emotional reserves.
At its core, IVF technology encompasses the complete process of ovarian stimulation, egg retrieval, and embryo handling, followed by embryo transfer into the uterus. This isn’t a single procedure but rather a coordinated series of steps, each requiring precise timing and technical expertise. What distinguishes modern IVF from earlier iterations is the integration of artificial intelligence, real-time monitoring systems, and predictive analytics that optimize every phase. Rather than relying solely on manual observation and experience-based judgment, today’s advanced clinics use machine learning algorithms to assess embryo quality, predict optimal fertilization timing, and personalize medication protocols based on your individual response. This technological leap has reduced treatment cycles from the typical three to six months down to approximately two weeks at facilities leveraging AI-driven protocols, a meaningful acceleration when you’re already managing the emotional weight of fertility treatment.
Several deeply ingrained misconceptions cloud the landscape of IVF technology. Many people believe IVF guarantees pregnancy or produces multiple embryos automatically, when in reality success rates depend on numerous biological factors, including egg quality and age-related decline in chromosomal health. Others assume that technology has made IVF safer and simpler than ever, failing to recognize that ovarian stimulation still carries real risks and requires careful monitoring. One particularly damaging myth suggests that AI and automation eliminate the human element of care, when the truth is that the complexity of treatment steps and patient variability demands constant human oversight and clinical judgment. Technology amplifies human expertise; it doesn’t replace it. Another widespread misconception portrays IVF as a last resort available only after years of failed attempts, ignoring that proactive fertility preservation through egg freezing and strategic timing of treatment actually improves outcomes considerably. Women frequently underestimate how their own knowledge of their cycle, response patterns, and medical history accelerates the process when paired with technology that personalizes care rather than applying one-size-fits-all protocols. The most consequential misconception, however, frames cost as fixed and unavoidable. Modern technology actually reduces unnecessary testing, eliminates redundant procedures, and prioritizes efficiency, bringing affordability within reach for far more people than traditional clinic models allow.
Pro tip: Request a detailed explanation of how your specific clinic uses AI in embryo assessment and treatment planning during your initial consultation, as the depth and sophistication of technological integration varies significantly between facilities and directly impacts both cost and timeline.
Here’s a comparison of traditional IVF versus AI-enabled IVF approaches:
Aspect | Traditional IVF | AI-Enabled IVF |
Embryo Assessment | Manual grading, subjective | Continuous, algorithmic, objective |
Treatment Duration | 3-6 months | Around 2 weeks |
Medication Protocols | Standardized, generic | Personalized, adaptive |
Outcome Prediction | Technician experience | Data-driven accuracy |
Cost Control | Multiple cycles, higher costs | Fewer cycles, reduced costs |
AI-Driven Embryo Scoring and Monitoring
Traditionally, embryo assessment relied on a lab technician peering through a microscope, making subjective judgments about cell division patterns, fragmentation, and symmetry at specific time points. This approach has inherent limitations: human fatigue affects accuracy, different technicians may score the same embryo differently, and you only capture snapshots rather than continuous development data. The real turning point came when fertility labs began integrating time-lapse imaging with artificial intelligence. Now, instead of static observations, embryos are monitored continuously in specialized incubators that photograph them every five to ten minutes for the entire development period. AI algorithms analyze thousands of these images, tracking morphokinetic markers (the specific timing of cell divisions and developmental milestones) with precision that human eyes simply cannot match. This shift from subjective assessment to objective, data-driven evaluation fundamentally changes how clinics decide which embryos have the highest implantation potential.
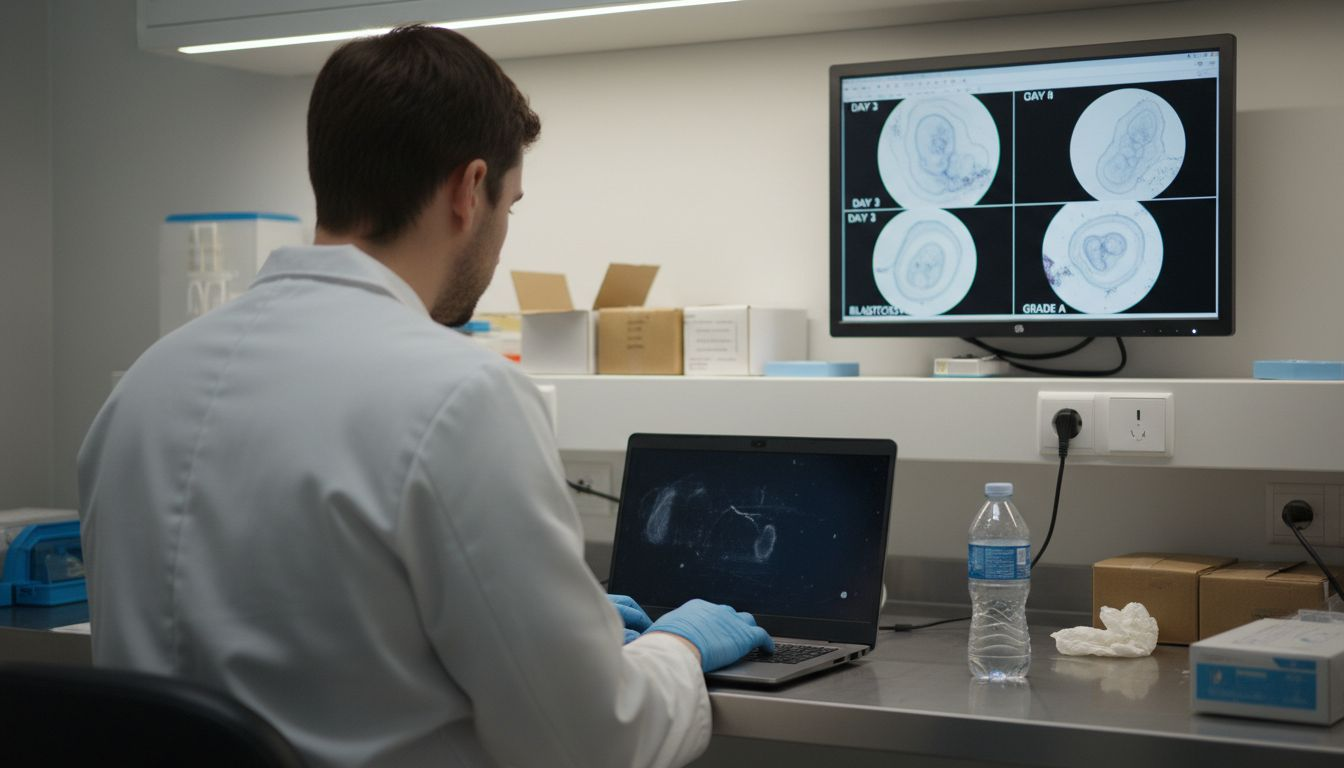
The accuracy improvements are striking. AI models for embryo quality prediction have reached up to 96% accuracy in identifying embryos most likely to result in successful pregnancies, compared to traditional morphology scoring alone which hovers around 70-80%. This matters enormously for you because it reduces the guesswork in embryo selection. Rather than transferring an embryo that looks promising under a microscope but carries hidden genetic issues or developmental problems, AI continuously monitors subtle indicators that predict true viability. The system flags which embryos are progressing optimally, which are developing too slowly, and which show chromosomal abnormalities long before they become apparent to human observation. Time-lapse imaging combined with deep learning for objective embryo assessment means your clinic can make smarter transfer decisions faster, reducing the emotional toll of uncertain outcomes and improving the probability that your first transfer succeeds.
What makes this technology particularly valuable for women under 40 with good ovarian reserve is the efficiency it enables. Rather than hoping your clinic grades your embryos conservatively or aggressively, AI applies consistent, evidence-based criteria across every single one of your embryos. This standardization accelerates decision-making because there’s no ambiguity about which embryos merit transfer versus which should be further monitored or frozen. Many women freeze multiple eggs expecting dozens of embryos, only to discover that traditional assessment methods discard far more embryos than necessary. AI-driven monitoring prevents this waste by identifying viable embryos that might otherwise be overlooked. Additionally, continuous monitoring captures critical developmental windows that conventional daily observations miss entirely. Cell division timings, pronucleus disappearance, and the precise sequence of cleavage events all predict implantation success far better than static morphology grades assigned once or twice daily. Your embryos are essentially being graded by an algorithm trained on thousands of successful and unsuccessful outcomes, calibrated to recognize patterns invisible to human judgment.
The practical advantage extends beyond accuracy into cost and timeline compression. When your clinic relies on subjective assessments, they often transfer multiple embryos to increase success odds, or they recommend additional testing and monitoring that extends treatment length. AI-driven protocols minimize this uncertainty, allowing single embryo transfer decisions that improve outcomes while reducing your financial burden and physical recovery needs. The technology also flags potential issues earlier, allowing your clinic to adjust treatment protocols in real time if needed rather than discovering problems after failed transfers.
Pro tip: Ask your fertility clinic whether they use continuous time-lapse monitoring with AI-assisted embryo scoring during your consultation, and request to see sample reports showing how their system grades embryos, as facilities using advanced monitoring often achieve higher implantation rates with fewer transfers.
Personalized IVF Protocols with AI
One of the most frustrating aspects of traditional IVF is the one-size-fits-all approach. Your clinic prescribes a standard stimulation protocol designed to work for average patients, but you are not average. Your age, BMI, ovarian reserve, hormone levels, and previous cycle responses all matter tremendously. A woman with exceptional egg quality at 35 needs a completely different medication dosage than someone at 38 with diminished ovarian reserve. Yet many clinics stick to the same starting doses and adjustment patterns for everyone, resulting in either overstimulation (leading to complications) or understimulation (resulting in fewer eggs than you actually could have produced). Personalized IVF protocols powered by artificial intelligence change this entirely. Rather than guessing at your optimal medication dosage, AI analyzes your individual medical profile, previous treatment data if available, and real-time hormone responses to recommend precise, tailored stimulation regimens that maximize your egg yield while minimizing risks.
The science behind personalization rests on understanding that P4 reproductive medicine (prediction, prevention, personalization, and participation) can be achieved by integrating large datasets from patient genetics, hormone profiles, and previous cycles. This means your clinic isn’t relying on static protocols developed decades ago or on one doctor’s clinical intuition. Instead, AI algorithms examine thousands of data points specific to you: your anti-Mullerian hormone (AMH) levels, follicle-stimulating hormone (FSH) baseline, body weight, age, and how you responded to hormones in any previous cycles. The system then predicts your optimal starting dose and creates a dynamic protocol that adjusts your medications throughout stimulation based on real-time ultrasound findings and hormone monitoring. If your follicles are developing faster than expected, doses decrease automatically. If growth lags, doses increase. This continuous optimization means you spend less time on medications, experience fewer side effects, and produce more viable eggs than you would under a fixed protocol. The time savings are substantial: personalized protocols can reduce stimulation duration from the typical 10-14 days down to 8-10 days, directly accelerating your overall treatment timeline.
What makes this approach especially valuable for women under 40 is the prevention of both undertreatment and overtreatment. Younger women often have excellent ovarian reserve, yet clinics sometimes start them on conservative protocols designed for older patients, resulting in disappointing egg counts that don’t reflect their actual fertility potential. Conversely, aggressive protocols in young women can trigger ovarian hyperstimulation syndrome, a serious complication that delays transfer and adds considerable cost and stress. AI-driven decision support tools tailored to individual patient data eliminate this guesswork by identifying the exact stimulation intensity that works for your body. The algorithms learn from millions of treatment cycles globally, recognizing patterns that predict how your unique physiology will respond. This precision extends beyond medication dosing into embryo transfer timing, progesterone supplementation, and even recommendations about whether to pursue a fresh transfer or freeze all embryos for later use. Some women benefit from transferring immediately after retrieval, while others achieve better outcomes with a frozen transfer allowing additional recovery time. AI analyzes your specific situation to recommend the approach most likely to succeed for you.
The financial impact deserves emphasis. Personalized protocols reduce wasted medication, minimize cycle cancelations due to poor response, and decrease the need for supplementary testing or repeat cycles. A woman who produces 18 eggs instead of 8 because her protocol was properly optimized has better odds of success in a single cycle rather than requiring two or three attempts. This compounds the cost savings: fewer cycles, fewer medications, fewer ultrasounds, and higher success rates all translate to affordability that makes fertility treatment accessible to more women. The emotional benefit is equally profound. When your treatment plan reflects your individual biology rather than generic guidelines, you feel heard and confident in the decisions being made. You understand why you’re taking a specific dose on a specific day, and you can see how your personal response data is guiding adjustments. This transparency and customization reduce the powerlessness many women feel during treatment.
Pro tip: Before starting stimulation, request a detailed written explanation of your personalized protocol including your specific starting dose, the criteria your clinic will use to adjust medications throughout your cycle, and the projected timeline based on your individual profile.
Streamlining IVF Pathways for Speed
The traditional IVF timeline feels interminable. You schedule an initial consultation, wait weeks for your appointment, undergo baseline testing, wait for results, adjust protocols, begin stimulation, monitor for two weeks, retrieve eggs, wait for fertilization reports, monitor embryos for five to six days, then finally transfer or freeze. The entire process stretches three to six months, and you spend most of it waiting. This extended timeline amplifies emotional stress, increases medication costs due to longer exposure, and for women under 40 with good ovarian reserve, it feels unnecessarily prolonged given that your biology is optimized for faster response. Modern technology fundamentally compresses this pathway. Advanced clinics now complete the entire cycle from initial consultation to embryo transfer in approximately two weeks by eliminating unnecessary delays, consolidating testing, and making data-driven decisions in real time rather than waiting for standard clinic schedules.
The speed acceleration comes from several synchronized innovations. AI and robotics for faster gamete and embryo handling reduce manual processing time while improving consistency and reducing contamination risk. Rather than a technician manually preparing samples and moving embryos through processing steps, automated systems handle these tasks with precision, freeing your clinical team to focus on decision-making and patient communication. Simultaneously, advanced predictive models eliminate the need for exploratory testing. Traditional clinics order extensive baseline blood work, imaging, and sometimes diagnostic procedures simply to understand your baseline status. AI systems trained on millions of patient profiles can predict your likely response category from minimal initial data, reducing unnecessary testing by 40 to 50 percent. This alone saves two to three weeks. Real-time monitoring systems that provide daily ultrasound and hormone results within hours rather than days allow your clinic to make protocol adjustments immediately, preventing the delays that occur when you wait until the next scheduled monitoring appointment to learn that your follicles are growing slower than expected. When your clinic can adjust your medication dose the same day based on hormone results rather than waiting three days for the next ultrasound, you progress faster through stimulation.
The speed advantage extends into the laboratory and decision-making phases. Traditional embryo assessment requires waiting until day five or six for definitive grading, then scheduling a transfer appointment, then potentially waiting again if the transfer is delayed by logistics or scheduling constraints. AI-enabled continuous embryo monitoring provides preliminary viability predictions by day three, allowing your clinic to flag problems early and adjust the plan accordingly. If only one embryo is developing normally, your team can discuss freeze-all strategies immediately rather than discovering poor quality on day five and then scrambling to change plans. Transfer scheduling becomes more flexible because AI predicts optimal timing rather than forcing you into standard day-five transfer windows. For some patients, day-three transfer actually produces better outcomes. Others benefit from waiting to blastocyst stage. The algorithm recommends the approach most likely to work for you specifically, eliminating the guesswork that often extends timelines.
What makes speed particularly valuable for your demographic is the preservation of ovarian reserve and egg quality. Every additional week of stimulation hormone exposure, every delayed cycle, and every unnecessary repeat attempt incrementally impacts your fertility trajectory. A woman at 37 with good reserve who completes IVF in two weeks rather than three months preserves biological advantage that matters considerably. The psychological benefit is equally important. Compressed timelines reduce the emotional toll of prolonged uncertainty and hope cycling. Instead of months of anticipation, you move through treatment efficiently, reach answers faster, and can make informed decisions about next steps with clarity rather than exhaustion. Financial impact compounds these benefits. Shorter treatment duration means fewer medications, fewer ultrasounds, fewer office visits, and fewer ancillary services, all contributing to affordability. A woman who completes treatment in two weeks instead of three months spends materially less money on the same outcome.
The speed optimization does not mean rushing or cutting corners. Rather, technology enables your clinic to compress unnecessary waiting time while maintaining rigorous medical standards. Every decision still rests on solid clinical data and medical judgment. The difference is that your clinic can access and act on that data immediately instead of processing it on a schedule designed decades ago when laboratory capabilities were more limited. You benefit from both the clinical advantages of modern protocols and the psychological and financial advantages of condensed timelines.
Pro tip: During your initial consultation, specifically ask your clinic about their average time from first appointment to embryo transfer, how they use AI to streamline decisions, and what their monitoring schedule looks like, since facilities with truly optimized pathways can articulate exactly how they compress timeline without sacrificing quality.
Cost, Risks, and Emotional Impacts
IVF carries real costs and real risks. No amount of technological sophistication changes that fundamental reality. What technology does change is the magnitude of those burdens and your ability to manage them with clarity and support. The financial cost of a single IVF cycle in the United States ranges from $12,000 to $25,000 depending on your location, clinic, and the specific services required. For women under 40 with good ovarian reserve, the goal is to achieve success in one or two cycles rather than four or five, making the total financial expenditure manageable rather than catastrophic. Yet traditional clinic models with extended timelines, unnecessary testing, and less precise protocols often require multiple attempts, compounding costs exponentially. A woman who completes her successful cycle in two weeks spending $15,000 faces a fundamentally different financial reality than someone who endures three failed cycles over nine months spending $50,000 total. Technology that streamlines pathways and improves success rates directly addresses this financial burden by concentrating resources into efficient treatment rather than spreading them across repeated attempts. Additionally, AI-driven protocols reduce medication waste and eliminate unnecessary procedures, bringing costs down by 20 to 30 percent for women using advanced clinics compared to traditional models.
The medical risks of IVF deserve honest discussion. Ovarian stimulation carries real complications. Ovarian hyperstimulation syndrome (OHSS) affects 1 to 2 percent of stimulation cycles and can range from mild bloating and discomfort to severe cases requiring hospitalization. Egg retrieval is a minor surgical procedure with small but real risks of infection, bleeding, and bowel or vessel injury. Pregnancy itself, whether achieved through IVF or naturally, carries inherent medical risks including miscarriage, ectopic pregnancy, and gestational complications. The multifaceted impacts of IVF include medical risks alongside financial and emotional dimensions that require honest assessment. What technology contributes is better risk stratification and prevention. AI algorithms identify women at higher risk for OHSS before stimulation begins, allowing your clinic to use modified protocols that reduce risk while maintaining efficacy. Real-time monitoring catches early warning signs of complications so your team can intervene before situations become serious. Continuous embryo monitoring identifies genetic abnormalities that would result in miscarriage, allowing transfer decisions that improve both success and safety. None of these technological advantages eliminate risk entirely, but they meaningfully reduce it by providing better information and faster response times.
The emotional dimension of IVF is where technology’s impact becomes most nuanced. Emotional and psychosocial challenges faced by IVF patients include stress from uncertainty, procedural burden, and financial pressure that extend across months of treatment. Each monitoring appointment brings anxiety about whether your follicles are growing adequately. Each fertilization report carries the weight of knowing exactly how many embryos survived, creating attachment to microscopic cells that most people will never see. Each day of waiting for results involves hope and fear intermingled in ways that exhaust you emotionally. Compressed timelines through AI-optimized protocols reduce this emotional toll by shortening the period of uncertainty from three to six months down to two weeks. Rather than months of liminal space where you are neither cycling nor pregnant, you move quickly through treatment and reach definitive outcomes. This speed alone provides psychological benefit. Simultaneously, technology enables better communication and support. AI-driven patient portals provide 24/7 access to your results and treatment progress, reducing the anxiety of wondering about your status and waiting for clinic staff to call during business hours. Personalized messaging through platforms like WhatsApp keeps you informed in real time and allows your clinic to reach you immediately if adjustments are needed rather than leaving you uncertain between scheduled check-ins.
What matters is approaching IVF with realistic expectations grounded in both the genuine benefits and genuine burdens of treatment. Yes, technology reduces costs and timelines and improves success rates. Yes, advanced monitoring minimizes certain medical risks. Yes, better communication reduces some emotional strain. But IVF is still medically intensive, still emotionally demanding, and still requires your physical and psychological investment. The women best served by fertility treatment are those who enter with eyes open to both the possibilities and the challenges, supported by clinics that combine technological sophistication with genuine empathy and robust mental health resources. Your age and good ovarian reserve are genuine advantages that technology can help you leverage effectively. But they do not eliminate the real nature of the journey you are undertaking.
Pro tip: Before committing to treatment, specifically ask your clinic about their OHSS prevention protocols, their mental health support resources, and their cancellation and refund policies, since these factors often matter more than the technology itself when managing the emotional and financial dimensions of IVF.
Key risks, emotional factors, and cost impacts in IVF treatment:
Consideration | Traditional IVF | Tech-Optimized IVF |
Risk Management | Higher OHSS, generic protocols | Early detection, tailored prevention |
Emotional Impact | Prolonged uncertainty, more stress | Shorter timelines, better support |
Financial Burden | Repeated cycles, increased costs | Fewer cycles, reduced spending |
Patient Support | Limited communication | Digital updates, real-time access |
Human Support in Tech-Enabled Fertility
Technology without humanity is cold machinery. You can have the most sophisticated AI algorithms, the most advanced embryo monitoring systems, and the fastest treatment pathways, but if you feel unsupported, unheard, and abandoned between appointments, the experience becomes hollow. The most effective fertility clinics understand that technology and human support are not competing priorities but rather complementary forces that together create the optimal experience. Your clinic’s AI can predict your optimal medication dosage with 96% accuracy, but a compassionate nurse who takes time to explain what that dosage means and why it matters creates the confidence that allows you to trust the process. Real-time monitoring systems can flag embryo development concerns within hours, but a reproductive endocrinologist who calls to discuss what you discovered together, answers your questions without rushing, and explores your options collaboratively turns data into meaningful care. Human expertise and compassionate care in fertility treatments remain critical to patient satisfaction and holistic care even as technology advances the clinical foundations of treatment. The technology should disappear into the background, working quietly to optimize your outcomes while your actual human interactions with your care team provide the support, clarity, and reassurance that make the journey manageable.
The ethical dimension of this balance matters profoundly. Fertility treatment involves profound decisions about your body, your finances, and your future family. These decisions cannot be made by algorithm alone. A machine can tell you that embryo A has a 78% implantation probability and embryo B has a 71% probability, but you need a human specialist who understands your medical history, your values, your financial constraints, and your emotional capacity to help you decide which embryo to transfer. Maintaining human involvement in assisted reproductive technologies ensures informed decisions and personalized support that algorithms simply cannot provide. You need to know not just what the technology recommends, but why your specific situation warrants that recommendation. You need to understand the risks and benefits in language that makes sense to you, not in statistical abstractions. You need to feel that your care team has actually considered who you are as a person, not just processed your data through a decision tree. The best fertility clinics use technology to enhance the efficiency and precision of care while preserving and prioritizing the human relationships that allow true informed consent and personalized medical judgment.
Practically, this means your ideal clinic combines technological sophistication with accessible human support. Automated monitoring systems should generate alerts that your care team reviews immediately, but a nurse should also call you to discuss what was found and what it means for your specific situation. AI-driven patient portals should provide 24/7 access to your results and progress, but your clinic should also offer real people available by phone, WhatsApp, or email to answer questions when you have them. Personalized protocols developed by algorithms should be reviewed by your doctor who can explain the reasoning and adjust based on conversations with you. Your embryos should be monitored by continuous time-lapse imaging, but your embryologist should take time to discuss what the images revealed about your specific embryos rather than simply handing you a grading report. Mental health support should be integrated into treatment planning, not treated as an afterthought. When your clinic recommends a freeze-all cycle instead of a fresh transfer, a counselor should help you process what that means emotionally and practically. When you receive a negative pregnancy test, your team should follow up to support you emotionally and discuss next steps, not simply leave you alone with your disappointment.
The transparency of this partnership matters enormously. You should understand exactly how your clinic uses technology and exactly what human judgment shapes your care. Some clinics use AI to make all embryo grading decisions and transfer recommendations. Others use AI to inform the analysis but preserve human embryologists and doctors who make final decisions. Neither approach is inherently right or wrong, but you deserve to know which one your clinic practices and to feel confident in the reasoning. Some clinics offer 24/7 communication through personal WhatsApp channels with your actual care team. Others offer portal access but require going through scheduling systems to speak with staff. Again, both models can work well, but you should choose based on what resonates with your communication needs and your sense of how supported you want to feel. The women most satisfied with fertility treatment are those who feel genuinely cared for by their clinical team, who understand their treatment plan completely, and who trust that both technology and human judgment are working in concert for their benefit. Technology accelerates and optimizes the medical aspects of fertility care. Human support makes the journey feel safe, personalized, and hopeful.
Pro tip: During your initial consultation, ask your potential clinic to explain not just what technology they use but how human specialists review and interpret that technology’s recommendations, and request examples of how they’ve used human judgment to modify AI recommendations based on individual patient circumstances.
Accelerate Your IVF Journey with Advanced AI-Powered Care
The journey through IVF should never feel endless or overwhelming. This article highlights the common challenges faced by women under 40 who want faster, personalized, and more efficient fertility treatment. From misconceptions about guaranteed success to the emotional toll of prolonged timelines, the pain points are clear. You want technology that not only improves embryo assessment with AI-driven monitoring but also tailors your medication protocols precisely to your biology. You deserve a fertility experience grounded in speed, accuracy, and human compassion.
At Aurea Fertility, we embrace the very innovations discussed here by integrating artificial intelligence throughout every step of your treatment. Our AI-enabled embryo scoring and personalized protocols condense the typical 3-6 month IVF cycle down to approximately two weeks. We minimize unnecessary testing and repetitive cycles while maximizing your chances of success. Plus, with 24/7 communication via WhatsApp and dedicated human support, you never face this journey alone. If you are ready to transform your fertility experience through smarter technology combined with genuine care, explore how our approach can meet your needs by visiting Aurea Fertility. Learn more about our AI-powered embryo monitoring and personalized IVF protocols.
Take control of your fertility timeline and emotional wellbeing today. Connect with Aurea Fertility now and experience fertility care that is faster, smarter, and truly personalized.
Frequently Asked Questions
What is the role of AI in IVF technology?
AI enhances IVF by providing data-driven insights into embryo quality, personalizing medication protocols, and predicting optimal treatment timing, ultimately improving success rates and reducing overall treatment time.
How does personalized IVF work with technology?
Personalized IVF uses AI to analyze individual patient data and hormone responses, allowing for tailored medication dosages and stimulation regimens that maximize egg yield while minimizing risks.
What benefits does AI-optimized IVF offer compared to traditional IVF methods?
AI-optimized IVF offers faster treatments, more accurate embryo assessments, personalized protocols, reduced costs, and improved outcomes through continuous monitoring and data-driven decisions.
How has technology reduced the timeline of IVF treatments?
Modern technology streamlines IVF by consolidating testing, utilizing automated systems for embryo handling, and providing real-time monitoring, cutting the overall treatment timeline from months to approximately two weeks.
Recommended

Comments